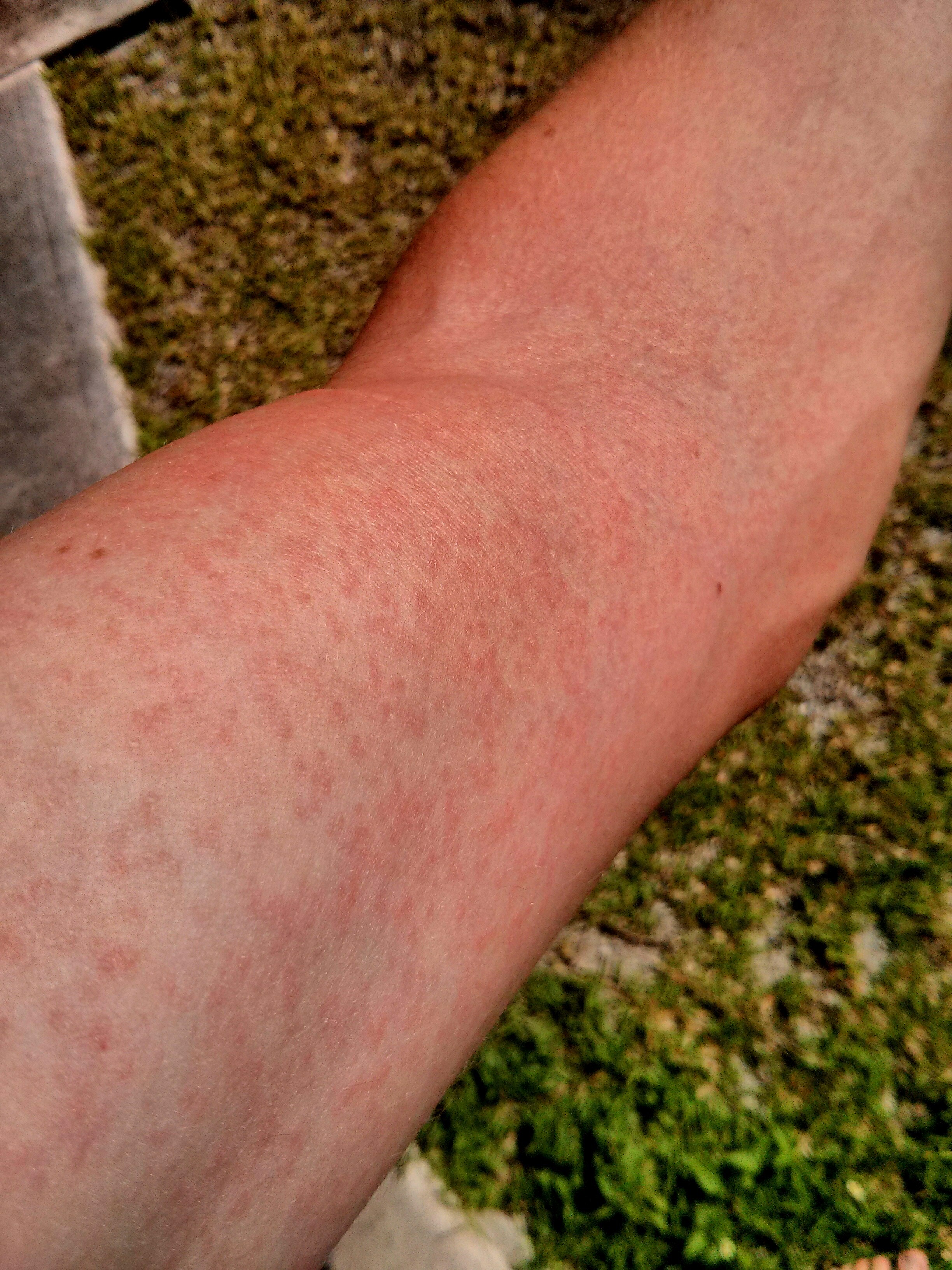
You're scrolling through Google Images, heart racing a bit, comparing a splotchy red patch on your arm to a dozen different zika virus rash pictures. It's stressful. Honestly, looking at medical photos online is a one-way ticket to anxiety-town because, let's face it, most red bumps look exactly the same to the untrained eye. But here’s the thing about Zika: the rash is often the loudest symptom of a virus that otherwise stays pretty quiet.
If you've recently traveled to a tropical climate or live in an area where Aedes mosquitoes are basically the unofficial state bird, you’re right to be curious. But don't just look at the color. You have to understand the behavior of the skin.
Zika isn't like a hive that pops up and disappears in an hour. It’s persistent.
The Specific Look of a Zika Rash
When we talk about zika virus rash pictures, we’re usually looking at something doctors call a "maculopapular" eruption. That’s just a fancy medical way of saying it’s a mix of flat red spots (macules) and tiny raised bumps (papules).
It starts. Usually on the face. Then it migrates.
Within a day or two, it spreads like a slow-moving wave down to the trunk, arms, and eventually the legs. It’s not usually shy. Unlike some viral rashes that hide in the folds of the skin, Zika tends to be quite visible on the limbs and torso. One of the most defining characteristics—and this is something you can’t always "feel" just by looking at a photo—is that it’s incredibly itchy for many people. According to clinical observations from the CDC and the World Health Organization, the pruritus (itching) is often the most complained-about part of the physical rash itself.
Wait, there's more.
The redness is often intense. It’s a "blanching" rash, meaning if you press your finger onto a red spot, it turns white for a second before the blood rushes back. If you’re looking at zika virus rash pictures and the skin looks bruised or like there are tiny broken purple blood vessels (petechiae), you might actually be looking at Dengue or Chikungunya instead. These viruses are transmitted by the same mosquitoes and often overlap in the same geographic regions, like Brazil or Puerto Rico.
Why Your Screen Might Be Lying to You
Here is the problem with self-diagnosing via a search engine. Most of the top-ranking images for Zika are extreme cases. They show the most "textbook" versions because those are the most educational. But in reality, Zika is a master of disguise.
Sometimes it’s faint.
If you have a darker skin tone, the rash might not look red at all. It might appear purplish, brownish, or just look like a change in texture. This is a massive gap in many online medical databases. A study published in The Lancet Infectious Diseases has previously highlighted how the lack of diverse skin tone representation in medical literature leads to misdiagnosis. So, if you don’t see a photo that matches your skin exactly, don't assume you're in the clear.
The rash usually shows up between 3 to 12 days after the mosquito bite. It’s rarely the only guest at the party. You’ll probably have a mild fever, joint pain (especially in the small joints of the hands and feet), and—the big one—conjunctivitis.
Red eyes. No goop.
If you have a rash and your eyes look like you’ve been up for 48 hours straight but they aren't "crusty" or leaking fluid, that’s a very strong clinical marker for Zika.
Distinguishing Zika from Dengue and Chikungunya
It's a "triple threat" situation in many parts of the world. Because these three viruses share the same vector, they often show up in the same neighborhoods at the same time.
- Dengue: This is the "breakbone fever." The pain is deep in the bones. The rash usually appears later in the illness.
- Chikungunya: This one is all about the joints. People are often bent over in pain. The rash is present in about half of cases but isn't always the main event.
- Zika: The rash is very common (appearing in about 90% of symptomatic cases) and the fever is usually lower than Dengue.
Basically, if you feel "kinda sick" but have a "really bad rash" and "red eyes," Zika is the primary suspect. If you feel like you’ve been hit by a literal truck and your fever is pushing 104°F, you’re likely looking at Dengue.
The Real Danger: It’s Not the Skin
We focus on the rash because it’s what we can see. But as anyone who followed the 2015-2016 outbreak knows, the real concern is what the virus does to a developing fetus.
Microcephaly.
This is why zika virus rash pictures are searched so heavily by pregnant women or couples trying to conceive. The virus has a terrifying ability to cross the placental barrier and attack the neural progenitor cells in the fetal brain. It doesn't matter if the mother's rash was mild or if she didn't have a rash at all. The severity of the skin reaction has zero correlation with the risk to the baby.
Also, it's sexually transmitted. That’s the curveball. Most mosquito-borne illnesses stay between the bug and the human. Zika stays in semen for months. This is why the advice isn't just "wear bug spray," but also "use protection" if you've been to an endemic area.
What to Do If You Have a Suspected Zika Rash
If you're looking at your skin and it matches the "splotchy, itchy, spreading" description, don't panic, but do be smart.
- Don't take Aspirin or Ibuprofen yet. This is a huge mistake people make. If it turns out you actually have Dengue, these NSAIDs can increase the risk of bleeding. Stick to Acetaminophen (Tylenol) until a doctor tells you otherwise.
- Hydrate like it’s your job. Viral infections tax your system.
- Get a NAAT test. This is a Nucleic Acid Amplification Test. It looks for the actual RNA of the virus in your blood or urine. It's most accurate in the first week. After that, you have to rely on antibody testing (MAC-ELISA), which is notoriously "sticky" and can sometimes give a false positive if you've had a yellow fever vaccine or a previous Dengue infection.
- Stop the spread. If you have Zika in your blood and a local mosquito bites you, that mosquito is now a carrier. You’ve just started a local outbreak. Stay indoors and use repellent even while you're sick to protect your neighbors.
The rash usually fades within a week. It doesn't typically peel like a sunburn, though some people report minor flaking as the inflammation dies down.
Navigating the 2026 Landscape
While the massive global headlines have faded since the mid-2010s, Zika hasn't gone anywhere. It’s endemic in many parts of Southeast Asia, Africa, and the Americas. Climate change is pushing Aedes aegypti and Aedes albopictus mosquitoes further north every year. We’re seeing more "locally acquired" cases in places like Florida and Texas than we used to.
It’s just part of the environment now.
If you are pregnant, the CDC guidelines remain pretty strict: avoid travel to areas with active Zika transmission. If your partner travels there, you wait. You wait months. It’s frustrating, but the neurological stakes are just too high to gamble on a "maybe" based on a few zika virus rash pictures you saw on a smartphone screen.
Practical Next Steps for Self-Assessment
If you are currently looking at a rash and suspect Zika, take these immediate actions:
- Check your temperature. A low-grade fever (around 100.4°F to 101°F) is a classic companion to the Zika rash.
- Look in the mirror. Check the whites of your eyes for "bloodshot" appearance without discharge.
- Trace the timeline. Did this start on your face and move down? How many days ago were you bitten?
- Document the rash. Take clear photos in natural light. This is much more helpful for your doctor than trying to describe "red spots" over the phone.
- Contact a travel medicine specialist. Regular GPs might not see Zika often. If you’ve recently traveled, mention your specific destination (e.g., "I was in the Petén region of Guatemala") to help them narrow down the specific viral strains active in that area.
The rash is a signal. It’s your body’s way of saying something is hitching a ride in your bloodstream. While the spots themselves are temporary and mostly just annoying, the implications for reproductive health and community spread are where the real focus should stay.
Stay covered, use DEET or Picaridin, and if the spots appear, get the bloodwork done to know for sure.