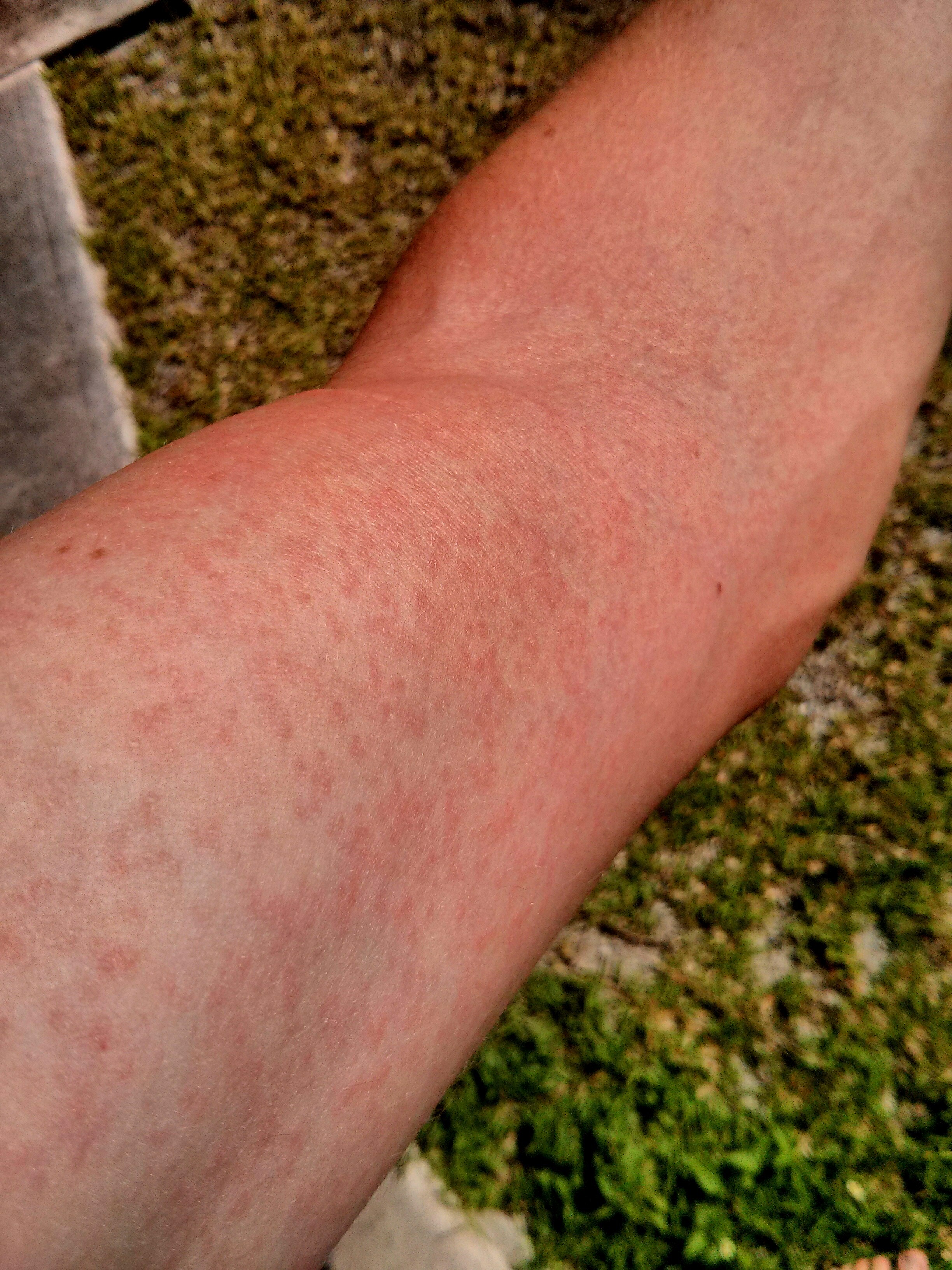
Finding a weird, blotchy breakout after traveling can be nerve-wracking. Honestly, if you’re looking up a zika virus rash photo, you’re probably trying to figure out if those red spots on your arm are just a heat rash or something way more serious. It’s tricky. Zika isn’t like the chickenpox where the blisters are unmistakable. It’s subtle, often itchy, and looks frustratingly similar to a dozen other tropical ailments.
Most people think of Zika as a "pregnancy virus," but the reality is that anyone can catch it. It’s spread primarily by the Aedes aegypti mosquito. You’ve likely heard of it. The same bug carries Dengue and Chikungunya. While the news cycle has moved on since the 2016 global emergency, the virus is still endemic in many parts of the world. Understanding what the skin manifestations actually look like is the first step toward getting the right care.
What a Zika Virus Rash Actually Looks Like
If you look at a confirmed zika virus rash photo, the first thing you’ll notice is the "maculopapular" nature of the breakout. That’s a fancy medical term doctors use to describe a rash that has both flat red spots (macules) and tiny raised bumps (papules). It’s not usually one giant welt. Instead, it’s a dense "carpet" of small, pinkish-red dots that can eventually merge together.
It usually starts on the face. From there, it travels. Fast. Within a day or two, it might spread to your trunk, your arms, and eventually your legs. A weirdly specific trait of Zika is that it often shows up on the palms of the hands and the soles of the feet. Most common viral rashes avoid those areas, so if you see spots there, take note.
The itch factor
Is it itchy? Usually, yes. It’s not "poison ivy" levels of intense itching, but it’s definitely bothersome. Some patients described it as a prickly sensation. Others say it feels like a mild sunburn that won't stop tingling. Interestingly, the CDC notes that the rash usually appears 3 to 12 days after the mosquito bite. If you just got bitten five minutes ago and have a bump, that’s just a local reaction, not Zika.
Why the Zika Virus Rash Photo is Often Confusing
Here is the thing about medical photos online: lighting changes everything. On lighter skin tones, the rash looks like a bright rose-colored blush. On darker skin tones, it might appear more purple or even brownish, making it much harder to spot unless you’re in direct sunlight.
The biggest challenge for clinicians is "The Big Three." Zika, Dengue, and Chikungunya all look almost identical to the naked eye. In a study published in The Lancet Infectious Diseases, researchers pointed out that because these viruses circulate in the same geographic regions, you can’t just look at a photo and diagnose yourself. You need blood or urine testing. Zika tends to have more prominent "conjunctivitis"—red, irritated eyes without discharge—compared to the others.
If your eyes look like you’ve been swimming in a chlorinated pool for six hours, and you have that sandpaper-textured rash, Zika becomes the primary suspect.
Beyond the Skin: Other Symptoms to Watch For
The rash is just the billboard. The real stuff is happening inside. About 80% of people who get Zika don't even know they have it. They have zero symptoms. For the unlucky 20%, the rash is almost always accompanied by a specific set of "friends."
- Joint pain: This is usually in the small joints of the hands and feet.
- Fever: It’s typically a low-grade fever. If you’re hitting 104°F, it’s more likely Dengue.
- Muscle pain: General achiness that feels like a mild flu.
- Headache: Often concentrated right behind the eyes.
According to the World Health Organization (WHO), symptoms generally last for 2 to 7 days. It’s short-lived, but the implications for certain groups are massive.
A note on pregnancy and risks
We have to talk about the elephant in the room. The reason we care so much about identifying a Zika rash is because of its link to microcephaly and other congenital brain abnormalities. If a pregnant woman identifies a potential zika virus rash photo that matches her own skin, she needs to contact an OB-GYN immediately. The virus can cross the placenta. It’s not just a "skin thing" then; it’s a neurological concern for the developing fetus.
Misconceptions About the Rash
People think the rash is the "scary part." It’s not. The rash is actually a sign your immune system is fighting back. A common misconception is that a bigger, redder rash means a more dangerous infection. That’s not true. The severity of the skin breakout doesn't correlate with the risk of complications like Guillain-Barré syndrome, a rare condition where the body’s immune system attacks the nerves.
Another myth? That you can catch Zika from touching someone else’s rash. You can't. It’s not contagious through skin-to-skin contact. It’s blood-borne and sexually transmitted. If you see someone with the rash, you aren't at risk just by being in the same room—unless there’s a mosquito in that room that bites them and then bites you.
Real-World Management: What to Do If You Have It
So, you’ve looked at the zika virus rash photo, checked your arms in the mirror, and you’re convinced. What now?
First, stop taking aspirin or ibuprofen. This is a crucial, often overlooked piece of advice. Because Zika looks so much like Dengue, and Dengue can cause bleeding issues, taking NSAIDs (like Advil or Aleve) can actually increase your risk of hemorrhaging. Stick to Acetaminophen (Tylenol) for the fever and pain until a doctor confirms it isn't Dengue.
Second, hydrate. It sounds like a cliché, but viral infections dehydrate the body quickly.
Third, prevent more bites. If a mosquito bites you while you have the virus in your blood, that mosquito is now a carrier. You’ve basically become the "source" for your neighborhood. Wear long sleeves and use DEET-based repellent even while you’re sick at home to break the cycle of transmission.
Testing and Diagnosis Limitations
You can't just walk into a local pharmacy and get a "Zika rapid test" like you can for COVID-19. It’s more complicated. Doctors usually use a PCR (Polymerase Chain Reaction) test to look for the virus's RNA in your blood or urine. This only works in the first week.
After the first week, they look for antibodies (IgM). But here is the kicker: the antibody test often "cross-reacts." If you’ve had a Yellow Fever vaccine or a previous Dengue infection, the test might show a false positive for Zika. It’s a bit of a diagnostic nightmare. This is why history matters—where you traveled and when the rash started is just as important as the lab results.
Actionable Steps for Recovery and Safety
If you suspect you are looking at a Zika rash on your own body, follow these specific steps to manage the situation effectively:
- Document the rash: Take a high-quality photo in natural light. This helps your doctor track the progression, as the rash changes quickly.
- Switch to Tylenol: Avoid all blood-thinning painkillers until Dengue is ruled out by a medical professional.
- Notify your partner: Since Zika stays in semen longer than in blood, use protection during sex for at least 3 months (for men) or 2 months (for women) after symptoms start to prevent transmission.
- Consult a Travel Medicine Specialist: General practitioners in non-tropical areas might not see Zika often. A specialist will know exactly which lab codes to order for the PCR test.
- Monitor for Neurological Symptoms: If you feel any tingling, weakness, or "pins and needles" in your legs that moves upward, seek emergency care. This could be the start of Guillain-Barré, which requires immediate hospitalization.
The rash itself will fade on its own. You don't usually need special creams, though an oatmeal bath or an over-the-counter hydrocortisone cream can help if the itching becomes unbearable. Most people recover fully without any lasting issues, provided they aren't in a high-risk group.
Understanding the visual cues is important, but it’s the systemic response—the fever, the joint pain, and the travel history—that completes the picture. Stay indoors, keep the mosquitoes away, and let the virus run its course while keeping your healthcare provider in the loop.